What Is Plantar Fasciitis?

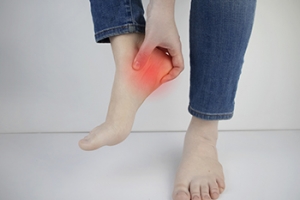
Plantar fasciitis is a common and often painful condition that affects the sole of the foot, particularly the heel area. It occurs when the plantar fascia, a thick band of tissue that runs along the bottom of the foot, becomes inflamed or irritated. The primary symptom of plantar fasciitis is intense heel pain, typically described as a stabbing sensation, especially during the first steps in the morning or after prolonged periods of rest. This condition is commonly associated with factors like excessive standing, walking, running, or wearing shoes with inadequate arch support. Treatment for plantar fasciitis often begins with conservative measures, such as rest and stretching exercises to alleviate inflammation and improve flexibility. Wearing supportive footwear and orthotic inserts can provide relief by reducing strain on the plantar fascia. In cases where conservative methods fail to provide relief, more advanced treatments such as corticosteroid injections, shockwave therapy, or night splints may be recommended. Surgery is considered a last resort for severe cases. If you have persistent heel pain, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment that is right for you.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Reasons for Swollen Feet During Pregnancy

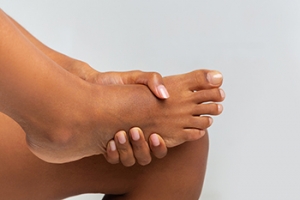
Swollen feet are a common companion to the miraculous journey of pregnancy, stemming from a combination of physiological changes and increased demands on the circulatory system. As the body nurtures a growing life within, blood volume surges, causing fluid retention in various tissues, including the feet. Hormonal shifts play a pivotal role, promoting relaxation of blood vessels and allowing for increased fluid accumulation. The expanding uterus exerts pressure on major blood vessels, hindering efficient circulation and contributing to swelling in the lower extremities. Prolonged standing or sitting can exacerbate this swelling, emphasizing the importance of regular movement and elevation of the feet. While edema during pregnancy is typically benign, it is essential to distinguish it from conditions like preeclampsia. If your feet become swollen during your pregnancy, it is suggested that you speak to a podiatrist who can offer you effective relief methods.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Pregnancy and Foot Health
Many pregnant women complain about foot pain while they are expecting. Foot pain can primarily be caused by weight gain and hormonal changes taking place in the body. By understanding how pregnancy impacts the health of a woman's feet, a pregnant woman can take action to keep her feet as healthy and comfortable as possible.
Because a woman's weight changes during pregnancy, more pressure is brought to bear on both the legs and the feet. This weight shift can cause two major foot problems: over-pronation, also known as flat feet, as well as edema, which is swelling of the feet. Over-pronation occurs when the arch of the foot flattens, causing the foot to roll inwards when the individual is walking, and can aggravate the plantar fascia tissues located along the bottom of the feet. If these tissues become inflamed, a pregnant woman can experience pain in the heel of the foot as well as severe foot pain while walking or standing. Swelling of the feet, or edema, often occurs in the later stages of pregnancy. It is caused by slow circulation and water retention, and may turn the feet a light purple color.
To keep feet in good health and prevent over-pronation, pregnant women should avoid walking barefoot and be sure they are wearing shoes that offer good arch support. A device known as an orthotic can be added to regular footwear in order to provide additional support for the feet during pregnancy. Any expectant mother whose feet hurt should first check to see if the shoes she is wearing are old, worn out and not offering the proper support necessary for distributing the weight of her body during pregnancy.
To treat edema of the feet, a good start is to wear quality footwear which offers support and good circulation. Keep feet elevated whenever possible by using a foot stool while seated. Stay well hydrated by drinking plenty of water to prevent water retention in the feet. Any swelling that occurs in only one foot should be examined as soon as possible by a doctor.
Good foot health during pregnancy can help expectant mothers avoid foot pain that leads to other health problems. Massaging the feet and doing regular gentle exercise like walking aids foot health by contributing to good circulation. Supportive shoes are also a good investment that will support foot health during pregnancy.
Common Sources of Foot Pain

For most people over the age of 50, foot pain is a common experience, affecting approximately 20 percent of older adults. Contributing factors include excess weight, inappropriate footwear, and the natural wear and tear associated with aging. However, it is essential not to dismiss foot pain, as research suggests it can compromise balance and foot function, and increase the risk of falls. Distinguishing between muscle soreness from activity and sharp pain originating from bones or joints is important. If experiencing the latter, seeking help from a medical professional is imperative. Several types of foot pain warrant such attention. Stress fractures, prevalent in older adults, manifest as pain during activity that subsides with rest. Persistent heel pain, such as plantar fasciitis, may require evaluation from a podiatrist if it persists despite rest. Psoriatic arthritis, characterized by joint pain and swelling, often accompanied by psoriasis symptoms, requires attention. Neuropathy, frequently linked to diabetes but with various causes, demands investigation for symptoms like tingling, burning, or foot numbness. If you are experiencing persistent or sharp foot pain it is suggested that you schedule an appointment with a podiatrist for a diagnosis and tailored treatment plan.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
Our feet are arguably the most important parts of our bodies because they are responsible for getting us from place to place. However, we often don’t think about our feet until they begin to hurt. If you have pain in your feet, you need to first determine where on the foot you are experiencing it to get to the root of the problem. The most common areas to feel pain on the foot are the heel and the ankle.
Heel pain is most commonly attributed to a condition called plantar fasciitis. Plantar fasciitis occurs when the plantar fascia, which is the band of tough tissue connecting the heel bone to the toes becomes inflamed. Plantar fasciitis pain is usually worse in the morning, and it tends to go away throughout the day. If you have plantar fasciitis, you should rest your foot and do heel and foot muscles stretches. Wearing shoes with proper arch support and a cushioned sole has also been proven to be beneficial.
Some common symptoms of foot pain are redness, swelling, and stiffness. Foot pain can be dull or sharp depending on its underlying cause. Toe pain can also occur, and it is usually caused by gout, bunions, hammertoes, ingrown toenails, sprains, fractures, and corns.
If you have severe pain in your feet, you should immediately seek assistance from your podiatrist for treatment. Depending on the cause of your pain, your podiatrist may give you a variety of treatment options.
Definition and Causes of Toenail Fungus

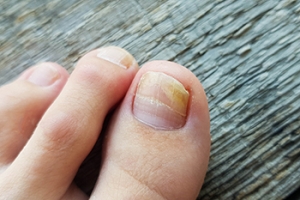
Onychomycosis, a common fungal infection affecting the nails, unveils itself as a condition that warrants a closer inspection. This ailment, known as a fungal nail infection, targets the toenails or fingernails, causing discoloration, thickening, and brittleness. The infection is often attributed to various fungal strains, primarily dermatophytes, but also yeasts and molds. These fungi thrive in warm and moist environments, making nails susceptible to infection when exposed to such conditions. Several factors contribute to the development of onychomycosis. Trauma to the nails, poor hygiene practices, and a compromised immune function elevate the risk. Additionally, communal spaces, such as public showers and swimming pools, serve as potential breeding grounds for the fungi, facilitating its transmission. If you have developed toenail fungus, it is strongly suggested that you confer with a podiatrist who can effectively treat this condition.
For more information about treatment, contact Brian D. Jackson, DPM of Neuhaus Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
Treatment Options for Stress Fractures

Treatment options for stress fractures focus on promoting healing, managing pain, and preventing complications associated with these injuries. Stress fractures typically result from repetitive stress or overuse and require careful attention to facilitate recovery. Rest is a fundamental component, involving the reduction or avoidance of activities that led to the fracture, allowing the affected bone to heal without additional strain. In some cases, immobilization with the use of casts, braces, or walking boots may be necessary to support proper healing. Modifying weight-bearing activities can also alleviate stress on the fracture site, often requiring the use of crutches or assistive devices. Pain management strategies may involve medications to address discomfort and inflammation. Wearing custom orthotic devices or shoe inserts may offer better support and alignment for the affected area, reducing bone stress. Adjusting activity routines, incorporating appropriate warm-up and cool-down exercises, and avoiding excessive exertion are essential in preventing future stress fractures. A balanced diet with sufficient calcium and vitamin D supports bone health and healing. While surgery is rarely needed, it may be considered when conservative treatments prove ineffective at stabilizing the bone. If you have sustained a stress fracture in your feet or ankle, it is suggested that you schedule an appointment with a podiatrist for an evaluation and personalized treatment plan.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot care needs.